Trigger warning: this chapter discusses some disturbing, emotionally difficult material.matic
Traumatic Incidents Affect Your Inner Mammal
I woke up in my bed at 5:15 a.m. to a bright flash of light and an explosion. It was the loudest sound I have ever heard. I could feel the force of the blast resound in my chest. At first, I assumed there was someone in my bedroom with a shotgun. I leaped out of bed for cover and then heard footsteps and yelling just outside my bedroom window. I didn’t know what to do. My home had been burglarized before, and I even experienced a robbery a few months prior, so I assumed I was experiencing a home invasion. After a half-hour of walking around maniacally with a baseball bat, I finally got the local watch commander on the phone. He told me police had served a warrant next door and used stun grenades to gain entry.
It had never crossed my mind that law enforcement caused the situation. As soon as I knew the explosions were not criminal, I started to calm down. At least the conscious part of me knew I was no longer in danger. On the other hand, my cat, Niko, couldn’t understand this. He engaged in all kinds of nervous behavior that I had never seen from him: looking over his shoulder, pawing at the ground, and shaking. I tried my best to calm him, but I didn’t know how to communicate to him that we were safe now. I got dressed and took the bus to work. There were no empty seats that morning, so I stood up, feeling the ice in my blood and the tremors shoot down my spine. Holding the rail, I asked myself: “How am I going to face my colleagues and give my talk this afternoon?” At the time, I knew next to nothing about diaphragmatic breathing, and hadn’t developed any Program Peace exercises, so I struggled through it. The audience could tell I was overwhelmed.
That night I couldn’t sleep. My conscious self knew I was completely safe. But, my unconscious brain areas—that, like my cat, don’t speak English—didn’t know this. Like small, scared animals, these brain modules continued to be emotional because they do not have access to the conscious, declarative knowledge that there never was any real threat. Evolution kept these brain modules in the dark because the organism cannot afford to trust the semantic belief that “I’m pretty sure I’m safe now.” You may not be able to talk to or reason with these modules, but you can communicate with them using your breath. Deep breathing persuades them to cool off. I didn’t have paced breathing back then to help me keep the trauma from sinking in, but I was able to use it years later to dig it out.
My overreaction to that situation was shaped by prior experiences. I have been violently assaulted several times in my life. I have been held up at knifepoint and seen people stabbed, shot at, and beaten. I have never received an official diagnosis, but I believe these experiences caused me to develop a form of PTSD, even if a subclinical one. Panicking didn’t help me in any of these situations. The heightened anxiety from one did not serve me in the next. The morning after, I would wake up with my teeth heavily clenched, eyes squinted into slits, lumbar spine contorted, and shoulders up around my ears. Many people suffer heinous traumatic incidents, much worse than these, that go on to desecrate modules throughout their body. I have a few friends that were “jumped” and beaten by groups of individuals. The neurological toll this takes can be ruinous, especially if it happens multiple times.
Car accidents, mugging, battery, rape, gruesome injury, childhood abuse, and anything that involves an incapacity to stop a terrible thing from happening can plant the seeds of trauma. Feelings of entrapment, immobilization, and helplessness make it worse. But it is when we allow these feelings to persist through time that the real damage occurs. Obsessive rumination, bracing, and distressed breathing occurring well after the actual event itself are what prime the body for suboptimality. These three things turn stress into trauma by “proving” to your unconscious that things have not gotten better. Alleviating them starts with the breath because if full, long, smooth, diaphragmatic, belly breathing does not resume, then your muscles won’t let it go, and your mind will continue to relive the tribulation. What traumatic episodes are you prolonging?
A Heightened Stress System
As discussed in Chapters 2 and 5, sustained stress changes the body’s life strategy. It convinces the body that the environment it was born into is particularly life-threatening. Scientists refer to such environments as high in “extrinsic mortality.” This kind of environment communicates to the organism on a cellular level that the probability of it being able to live a long and happy life is low. The genes then reprogram the body to deal with a short and grisly one. This changes your mortal shell from a slow-burning candle into a firecracker. Your body expends all its energy upfront because it doesn’t expect to live for long. This happens at the expense of long-term energetic investments such as healing, the immune system, learning, reproductive functioning, affiliation, and investing time and energy in offspring.[1 For example, chronic anxiety inhibits your body’s ability to protect itself from oxidation, which is a process that acts on your cells in the same way that rust acts on metal. It also contributes to aging by keeping the body from repairing its telomeres, the protective caps at the end of your chromosomes, reducing the number of times your cells can divide.
As you know, when stress goes on for too long, it results in a chronically heightened fear and startle response. The brain is retuned to enhance performance during life-threatening situations2 and facilitate cautiousness and hypervigilance, traits that would have been highly adaptive during extended periods of dire stress in prehistoric environments.3 These changes cause the stress response to become more pronounced and more easily triggered.4 The brain center that triggers stress, the amygdala, has its own innate response pattern to chronic stress. Let’s learn more about this almond-sized nucleus that acts as yet another biological repository of trauma.
The Amygdala Recognizes Threats
As we learned in Chapter 7, threats are recognized by the amygdala. This unconscious, subcortical area becomes active once it perceives a stimulus, or a group of stimuli together, as dangerous. The amygdala responds quickly and automatically to the inputs it receives from the eyes, ears, and other sense organs.5 If the threat is sufficient, it broadcasts the fear signal to the rest of the brain. It can do this unconsciously (a glimpse of a looming object), or visually (the view of a bus barreling toward you). The recognition of an abstract stressor (knowledge that you missed your bus) involves the prefrontal cortex, which indirectly alerts the amygdala.6 Either way, once the amygdala is activated, it will signal the hypothalamus which initiates fight or flight.

Illustration 21.1: A. Cross section of the brain with amygdala revealed. You actually have two amygdalae, one in each cerebral hemisphere; B. Three fear pathways to the amygdala: 1. The unconscious pathway travels from the eye to the thalamus, to the amygdala. 2. The visual pathway travels from the eye to the thalamus, to the visual cortex, to the amygdala. 3. The thinking pathway travels from the prefrontal cortex to the amygdala.
If the amygdala is strongly and repeatedly activated over the course of several weeks, its default level of activity will increase. Over months of repeated activation, the amygdala develops stronger connections with other brain areas intensifying its influence. It also increases in overall size.7 This enhanced priority given to the amygdala causes the animal to react to every seemingly threatening stimulus as if it were a full threat.
The amygdala’s job is to decide whether a pattern of inputs looks like something that turned out badly in the past. However, it does not use reason or conscious deliberation to do this. Rather, it engages in simple pattern matching in which it adds up seemingly bad inputs to see if they sum to a threshold. If the inputs surpass this threshold, the amygdala triggers the sympathetic nervous system. Thus, our feelings of dread are not prompted by logical thinking. Instead, they are initiated by the amygdala’s eccentric way of determining statistics and probability. For example, an offender’s voice, clothes, name, or cologne could subliminally reinstate an amygdala highjack.
Allow me to provide an example of how the amygdala’s form of logic is susceptible to mistakes. One day when I was in a lousy mood, I picked up the phone and the caller asked to speak to my roommate. The next day when I heard their voice again, it made me angry and I realized my prior bad mood had biased me against the caller for no good reason. Because my brain made this unconscious negative association, hearing the voice later triggered the same negative emotions. It was illogical and unfair to the caller. But my first impulse was to trust it unquestioningly. We accept the amygdala’s alarm bells as a type of foreboding intuition. Negative emotions usually feel valid and impelling, but they are often invalid and illusory. This is why we should question them rather than act on them impulsively. Especially after you experience a series of stressors, the amygdala will influence your thinking to be delusionally negative.
When activity in the amygdala surges, the brain is temporarily retuned to perceive everything as troublesome. For instance, it increases the tendency to perceive ambiguous events as bad, such as criticism when none is intended or hostility from a neutral face. This is the opposite of a manic episode, which causes people to perceive everything as a gleeful, lucky coincidence. People with mania often feel like cars on the freeway move to let them through, everyone is their best friend, and everything goes their way. On the other hand, chronic stress makes us more likely to succumb to road rage and the feeling that everyone and everything is against us. Whenever I start to feel disheartened, I try to remember that neurochemicals can paint over reality.
You may have noticed that after one negative interaction, you are much more likely to get stressed out about other, completely unrelated things. With the exception of living in a warzone this displaced negative thinking is irrational in the modern world. Interestingly though, it may not be irrational from an ecological standpoint. It was beneficial for mammals to be prepared for the worst during bad times. Just imagine what life would have been like for early mammals in the Jurassic and Cretaceous periods.
When there are predators on the loose or natural catastrophes strike, they are rarely quickly resolved. For furry varmints from possums to porcupines to panthers, it makes sense to become scared and remain paranoid. From a modern perspective, however, it is preposterous to generalize anxiety to whatever your mind turns to. Don’t let one unfortunate scenario lead to a domino effect of suspicion and dismay. Notice when you carry negative emotions from one thought over to another. When you realize it, try to tell yourself that the negativity may feel compelling but that it is probably just residual and misattributed emotion.
Stress and Cortisol: The Mind-Body Connection
“Stand porter at the door of thought. Admitting only such conclusions as you wish realized in bodily results, you will control yourself harmoniously.” — Mary Baker Eddy
When the amygdala decides it has perceived a stressful stimulus, it triggers the hypothalamus. The hypothalamus mobilizes the sympathetic nervous system, leading to rapid breathing, tense muscles, reduced sensitivity to pain, suspension of digestion, and a rise in heart rate and blood pressure. It also activates the adrenal glands, prompting the release of adrenaline. The release of adrenaline is a fast-acting hormonal response to an acute stressor. Adrenaline frees up blood sugars to give muscles and other tissues the energy they need to deal with an immediate threat.
After adrenaline, the second principal stress hormone is cortisol. Cortisol a is slow-acting response to a persistent stressor also released by the adrenals. It gives animals extra strength by liberating the energy from fat molecules into the bloodstream. This sounds like it could lead to weight loss, but it doesn’t. In the long run, cortisol promotes fat storage and muscle protein breakdown. It also changes the expression of several genes in fat tissue, increasing the likelihood of obesity and type 2 diabetes.8

Illustration 21.2: A. The kidneys with the adrenal glands sitting on top; B. The molecular structure of the hormone cortisol; C. The heart and lungs.
Chronic stress upregulates this entire stress hormone system, also known as the HPA (hypothalamic-pituitary-adrenal) axis. The result is that the body is continuously flooded with adrenaline and cortisol. Sustained elevation of cortisol is highly pathogenic and leads to hypertension, elevated heart rate, increased circulating levels of lipids and cholesterol, atherosclerotic plaque formation, decreased high-density lipoprotein (HDL) and increased low-density lipoprotein (LDL) cholesterol.9 Cortisol makes stress corrosive and is related to disorders like arthritis, asthma, acid reflux, cardiovascular disease, chronic fatigue, decreased metabolism, depression, various cancers, migraines, sleep deprivation, immune system impairment, and ulcers.10
Elevated cortisol also causes the immune system to produce inflammatory chemicals (cytokines). This results in inflammation (redness, warmth, and swelling), which increases the immune system’s ability to heal wounds from physical attacks. Again, this would have been advantageous in prehistoric times when stress indicated that cuts and lacerations were likely. In modern times however, chronically elevated inflammation can lead to pain, poor digestion, cancer, autoimmune disorders, and other dire disease states.11 In fact, it has been found to be a player in almost every chronic disease. To escape chronic inflammation, we must stop thinking inflammatory thoughts. But unfortunately, cortisol also acts on the brain.
Cortisol causes mammals to search desperately for a way out. Today, this urge to escape drives us to drink alcohol, smoke, overeat, and displace work-related frustrations on family members. If you are curious to see what highly elevated cortisol feels like, try submerging your entire forearm in an ice bath for two minutes. The pain from the ice causes a rapid spike in cortisol release, and this method is often used in experimental studies. When cortisol is raised like this, it causes subjects to perform mental tasks less flexibly and intelligently. It also increases pessimism, aggression, and the negativity bias.
As you might have guessed, elevated cortisol is common in humans and animals on the bottom of the pecking order. Cortisol is the hormone of status defeat, and it surges in monkeys and apes that are being dominated. Decades of studies on early life exposure to cortisol in monkeys reinforces much of what we have been discussing in this book. Exposure to trauma and cortisol makes a young monkey more psychologically vulnerable to stress and leads to decreased dominance, increased aggression, decreased social competence, reduced ability to find social interactions rewarding, and reduced affiliative drive.12 When we feel defeated, our serotonin and testosterone drop and our cortisol rises. Intermittent stressors like workplace abuse or even replaying uncivil incidents in one’s mind elevate cortisol levels.
Stress expert Robert Sapolsky wrote an excellent book on the neurobiology of stress called Why Zebras Don’t Get Ulcers. In the book, Sapolsky explains that most animals, other than social primates, do not give themselves ulcers because they don’t waste time worrying. Zebras, and most other animals, only get upset when they find themselves in immediate danger, usually involving a predator. If we only got upset when wild carnivores were stalking us, we would all be a whole lot happier! Moreover, zebras probably don’t rehearse negative social situations or mull over their place on the social ladder. It is mostly monkeys, apes, and humans that repeatedly model these scenarios in their heads. As a primate, your amygdala is inclined to latch on to social confrontation and cause it to be played out continuously in the imagination. This results in an existential nightmare that Chapter 7 offered you tools (e.g., nonjudgment, nonresistance, and nonattachment) to wake yourself up from. Most of these tools influence the way you assess problems.
The way you appraise a stress-provoking stimulus will program your automatic response the next time you encounter a similar stimulus. In other words, your brain will do its best to remember how you responded so it can expedite that response next time. So, when something alarms, shocks, or unpleasantly surprises you, don’t get caught up in it. Instead, try to immediately minimize the negativity.
Whether it is a mosquito whining in your ear, a car honking at you, or a person yelling at you, stop, take a deep breath, and choose to be calmer. Underreacting inoculates the amygdala against stress. Face difficulty with a levelheaded mindset that is as centered, grounded, and poised as possible.

Don’t Develop an Unhealthy Fear of Stress
“He who fears he shall suffer already suffers what he fears.” — Michel De Montaigne (1533-1592)
After recounting so many of the physical costs of stress in this book, I would be doing you a disservice if I didn’t encourage you not to stress out over stress itself. Here is why: Studies have shown that the pathogenesis of physical disease in response to stress is made much worse when someone believes that stress affects their health. Basically, thinking that stress is unhealthy makes it more unhealthy.13 Also, people who report they actively avoid stress are more likely to suffer from depression. So, what can we do?
When you feel stressed, don’t hate it, fear it, or fight it. Appraise it as enthusiasm and allow diaphragmatic breathing and belief in yourself to take away the unhealthy elements. Whenever you believe that you will end up stronger from a stressful incident, you almost always will. This is known as post-traumatic growth. People who see stress as normal and an opportunity for progress fare better. For instance, nervous public speakers who said, “I am excited” were rated as having better speeches than people who said “I am calm.”14 So, decide to see yourself as scrappy, full of grit, and able to bounce back. Believe that stress and arousal will create an advantage for you.
A stressor itself is inherently neutral. It is the way it is appraised that induces either distress or eustress. Eustress is positive stress and comes about when we decide we can cope successfully. Eustress, mounted in response to exciting challenges, drops off quickly rather than lingering like the cortisol response does.
Besides this distinction between distress and eustress, scientists also differentiate between the threat and challenge responses. The threat response is the fight-or-flight response that makes you angry or fearful, priming you for self-defense. The challenge response gives you initiative, helps you focus, and motivates you to confront obstacles. Both responses share several physiological factors, such as an increase in heart rate. However, when you feel challenged, your heart beats stronger, not just faster, giving you more energy.
During the threat response, the body is anticipating physical harm and makes relevant alterations. For example, blood vessels constrict to minimize blood loss due to injury sustained during combat. The body also increases inflammation and mobilizes immune cells to prepare for bruises and cuts. The threat response leads to cortisol and feelings of self-doubt. Studies have shown that, over time, the threat response leads to obesity, brain volume loss, and an increased risk of cardiovascular disease.15
The challenge response doesn’t do these things. The challenge response leads to tenacity and enthusiasm. Experts say that if you feel you don’t have what it takes to meet a situation head on, you experience a threat response. I agree. I also think that the threat response is selected when distressed breathing predominates and that the challenge response is selected when diaphragmatic breathing is retained. Use your deep breathing skills to turn threat responses into challenge responses.
I would also be remiss not to mention that low to moderate stress levels are natural and beneficial. In fact, most excitement is accompanied by a little adrenaline and cortisol, along with an increase in heart and breathing rates. We need some stress, just like we need to contract our muscles regularly. The problem with the stress response is when it is elevated chronically like a braced muscle.
I am asking you to avoid mulling over threats, fights, and abuse. I am not, however, asking you to deny reality or stop thinking about rising to meet challenges. Avoiding what makes you anxious can suspend growth. This is why it is important to expose yourself incrementally to gradations of challenging social situations. Voice that extra comment, joke, or observation to your peers to challenge yourself without pushing yourself into panic. Spark a conversation with a stranger. Chat up the clerk at the cash register. Find progressively larger audiences to share your ideas with and make eye contact for those few extra seconds. Every time you meet a moderate challenge and succeed, you become able to face bigger challenges. Assert yourself in ways you were hesitant to previously and push yourself to gently expand your comfort zone boundaries.
Remember those monkey studies we discussed a few sections back? It turns out that if the young monkey was exposed to elevated levels of cortisol a few times, but only briefly, then they developed increased resilience to stress and lowered cortisol levels. It toughened them up. Your stress system is just like a muscle, you want to push it through its full range regularly, but not for extended periods. Undergoing stress that challenges your cardiovascular and sympathetic system ends up being excellent exercise if you are not defeated by it and if you can relax afterward. Envision your stress system as agile and able to go from 0 to 100 and back to 0 uncomplicatedly. Endure, prevail, and recoup. Be made better and stronger by everything that happens by remaining fundamentally unharmed.
Feelings of Control and Safety
An animal’s stress is exacerbated when it cannot figure out how to make things better, feels helpless or powerless.16 A rat subjected to small electrical shocks will liberate significantly less cortisol if it thinks it has some control over the frequency of the shocks. Tricking the rat into thinking that pushing a lever reduces these shocks helps it remain calm, even if the lever actually does nothing.17 In a similar experiment, when a beeping noise preceded a shock to a rat’s foot, those rats had less severe ulcers than those with no warning. Because the stress had some predictability, the rats could retain a sense of control.
The moral of this story? Don’t focus on the elements of disturbing events that are unpredictable or uncontrollable. More importantly, know that your reactions, attitude, and reasoned choice are always under your control. Your breathing is always under your control as well. We all have times we are confused and uncertain. Do not let the nonlinear, chaotic, or unforeseeable distress you. Instead, take the time to identify which aspects of an unpleasant situation are malleable. This can help take the sting away from the unruly and erratic and help you turn threats into challenges.
Challenging yourself and embracing disorder is great, but there are times when you must feel able to completely put down your guard so that you can rest deeply. After the police loudly arrested my neighbor, I felt helpless in my own bed. This is not ok. Do what you must to make sure that you feel in control underneath your sheets, even if it means installing an alarm system or a thicker bedroom door with a deadbolt. The place where you sleep should provide sanctuary and refuge so you can debrace, recharge, and think safe, happy thoughts. The Buddha sat and slept at the base of the Bodhi Tree because it provided protection and security. He trusted it to have his back. Make sure your resting place makes you feel unconditionally secure.
Preventing Scalp Soreness and Other Forms of Hypoperfusion
Hair loss can be caused by stress. I have a friend who left his ferret alone for two days and came home to find it covered in bald patches. It is common for mammals to lose fur after trauma. The details are unclear, but it may be some kind of social signal. When chronic stress causes hair loss in humans, it is known as telogen effluvium. I started rapidly losing hair at the end of 11th grade. At the time, I had no idea what caused the sudden hair loss. Looking back two decades later, it is clear that it started immediately after having my nose broken. I believe the hair loss was a direct response to some form of high-intensity bracing that I took on after the injury that caused an outpouring of cortisol.
It is cortisol that makes hair follicles thin and fall out (it is also stress hormones that make them turn gray). This is why hair loss is associated with other stress-related illnesses like coronary artery disease, hypertension, dyslipidemia, and increased mortality.18 Although genetics plays a role in hair loss, abrupt hair loss from an early age is usually caused by extreme stress. By age 30, my hairline had receded to the midline of my scalp, farther than my father or grandfathers’ hairlines. Fascinatingly, my hair loss stopped (for eight years at least) immediately after I started paced breathing. Of course, only a little of my hair grew back because the miniaturization of the follicle responsible for balding is irreversible.
Another contributor to hair loss is reduced blood supply to the scalp. Stress and aging can reduce circulation and vasculature in subcutaneous tissues all over the head. This can cause scalp soreness. In the medical literature, sore scalp has been closely associated with hair loss (alopecia and male pattern baldness). I believe that you can reduce your risk of hair loss by increasing circulation in your scalp. Does your scalp feel sore when you firmly press a knuckle into it with five pounds of pressure? It shouldn’t. If it does, it may have reduced blood flow and the accompanying reductions in oxygen and nutrients. If the exercise below feels sore or painful, you should do it often to improve circulation. The intervention is simple, quick, and can vastly reduce scalp soreness in less than two weeks. Do the following:

When I started, five pounds of pressure from a single knuckle at the top of my head provoked unbearable discomfort. The sheer amount of pain suggested to me that the scalp is another anchor for trauma. So, I felt compelled to try to get the pain out. Within 10 five-minute sessions of the exercise above it went from puffy and dimpled with inflammation to smooth and sleek. Aside from the scalp there are other areas without underlying muscle that can be affected by poor circulation.
I often use headphones to listen to audiobooks when I take walks. After a few years of this, my ears hurt every time I took off my headphones. They were so painful one day that I figured I would have to stop wearing them. Frustrated with this, I cupped my palms over my ears and bent them forward firmly. This stung, so I spent 60 seconds bending them in different directions. It ached, but it also felt good. When I wore headphones the next day, it was much less painful. Three more sessions like this, and the pain was gone completely.
With age and uneven use, our tissues develop a condition called hypoperfusion. This is also known as diminished blood flow and is the reason my ears hurt. Reduced perfusion of blood can cause pain all around the body. As you know, pain exacerbates stress and drives the production of cortisol so we should be finding these areas and massaging them.
Hypoperfusion develops when tissues and organs receive reduced circulation due to diminishment in the number of small blood vessels. Pinching and bending my ears for less than five minutes overall provided the mechanical deformation of the tissues necessary to stimulate the creation of new small blood vessels (angiogenesis). All our hypoperfused tissues, including dormant muscles, need this kind of tender loving care. If it aches and itches, target it further. I want to encourage you to use compression, percussion, and vibration to address hypoperfusion anywhere you can find it because it will scale down your stress.
Drug Use Leads to Frailty and Chronic Distress
In my early twenties, I had between one and five alcoholic drinks on weekends, a cigarette every Saturday night, and a cup of coffee most weekdays. I wanted to stop, but I couldn’t help myself. When I was taking them, the drugs created the illusion of helping manage my stress. Taking them leads to relief because they mitigate distressed breathing for a few minutes, but in the long term, they actually contribute to it. It took me years to realize that even these uncontrolled substances lead to compulsive use, relapse after abstinence, and physical dependence.
Both nicotine and alcohol create a sense of euphoria that lasts a few minutes. However, the accompanying withdrawal from even a single use can lead to minor dysphoria that lasts days. Whether you are aware of it or not, this discomfort affects you emotionally and increases your bracing, shallow breathing, and emotional distress. I never noticed the withdrawal symptoms in my twenties, but after developing sensitivity to my inner states (discussed in depth in the next chapter), they became very apparent. Alcohol withdrawal symptoms include irritability, fatigue, shaking, sweating, nausea, headache, and difficulty concentrating.19 But these symptoms don’t just affect alcoholics who go cold turkey. They affect everyone who uses alcohol in a dose-dependent manner. The symptoms of smoking cessation can be worse. Withdrawal from any drug robs a user of diaphragmatic mobility, and I believe the resulting shallow breathing is a primary mechanism in addiction.
When you use psychoactive drugs every week, you experience fiendish cravings. I realized that two shots of liquor made me feel fearless for thirty minutes, and a cigarette extinguished my anxiety for an hour, but for the next few days, the subtle pain from withdrawal made me slightly more introverted and submissive. Situations that I would consider to be minor hassles before became calamities that would make me think, “My God, I’ve got to have a drink.” When you feel you “need” a cigarette is precisely when you shouldn’t smoke. Instead of masking the pain, work through it by spending some time with your breath metronome.
Intense social interactions that go on too long create loads of tension. Drugs amplify this. This is why after mixing the two, otherwise known as partying, you wake up feeling achy and nauseous, with a headache and stiff breathing. It is also why rock stars and child actors often burn out so fast. You cannot consume caffeine, alcohol, tobacco, or marijuana and hope to keep your latent trigger points from flaring up in social situations. Instead, intoxication makes you intensify your social displays without awareness of the increase in bracing.
When people use drugs recreationally, it makes them feel immune to social stress for a short time. This inevitably leads them to go too hard on their bodies. It proceeds like this: as you work the room, you strain your trigger points and chakras to the limit until you reach the point of needing another drink or cigarette. Using dulls the discomfort and allows you to continue to push your chakras, further deranging and abusing them. Soon, you are in so much discomfort that you’re turning to a third drink, a fourth drink, or possibly even harder drugs.
I thought I would always crave cigarettes and alcohol, but diaphragmatic retraining abolished my urges. In fact, studies have shown that paced breathing can help addicts maintain sobriety.20 Cigarettes and alcohol brought so much relief to me before but no longer did once I started breathing diaphragmatically. I believe that this is simply because there is little to relieve now. Instead, cigarettes generally just make my body feel weak, while alcohol makes me feel slow and tired.
There is a growing community of people who believe they can use drugs to achieve spiritual (entheogenic) growth. Sadly, almost all these people are oblivious to their shallow breathing while doing drugs. For this reason, most heavy trips are bad trips, even if the person does not realize it. I believe that if you want to do drugs, you should only do them while paced breathing. Otherwise, they will inevitably increase the extent of bracing going on under your level of awareness. Drugs should be used exclusively under the condition of complete composure. Under any other circumstances, they will unhinge your emotional well-being. However, hypocritically, I do recommend you take a drug for the following exercise.

Several drugs, including hallucinogens, dissociatives, and psychedelics, can induce temporary psychosis. Profoundly disturbing states of nightmarish terror, fear of overdose, or “ultimate entrapment” are commonly reported. A bad trip is not physical and emotional pain caused by a drug. It is preexisting pain from bodily tension and latent trigger points unmasked by the drug. Being exposed to this and being badly and unmindfully distressed by it increases trauma in the body. However, I think that any bad trip can be reversed by 30 minutes of paced breathing. Mental health specialists are searching for a treatment that can be administered to patients shortly after an overdose, panic attack, or horrific trauma. I believe that deep, paced breathing should be used in emergency response and clinical settings because it has the power to terminate these states and, in so doing, help block the formation of traumatic memories.
I have a friend who smokes concentrated THC every day, smokes cigarettes hourly, and drinks between 10 and 15 drinks a night, every night. This sounds like a living hell to most people. But few realize that doing less than this is just a proportionately smaller version of that hell. I have watched this woman’s good looks erode over just a few years. Every time I see her, the squinting and sneering are further entrenched. She doesn’t even do any hard drugs, but the poor gal is in constant displeasure and dissatisfaction driven by her withdrawal symptoms. She once described her pain to me as claws and teeth, tugging at her internal organs and devouring her from the inside out. I believe this is an insightful description of what it feels like to have your chakra-like modules saturated in inflammation and trapped in partial contraction.
Video Games, Violent Movies, and Loud Music Contribute to Stress
Humans have a tendency to create unhealthy attachments to forms of overstimulation. I was addicted to video games, violent movies, and loud music. Just as with drugs, we become hooked on the dopamine and adrenaline they produce, and the fleeting thrill causes us to ignore the persistent, low-level panic.
Traditional hunter-gatherers had exceptionally low stimulation levels 95% of the time. They were out in nature. Today, we plug into many streams of overstimulation that promote thrill-seeking and hyperarousal. Videos of street fights, “epic fails,” people getting injured, combat sports, horror movies and other forms of sensory assault are some of the most popular videos online. As with pornography, these intense but damaging experiences make us dissatisfied with our real lives. I believe that some people’s limbic systems respond to intense media stimulation with the challenge response, but I think most respond to them with the threat response.
Social media use, video games, and the violent nature of modern movies and television fragment our attention and foster a gambling mindset that causes us to become addicted to short-lived thrills. News outlets design the daily coverage of current events and politics to incite negative emotions because it grabs attention. Everything from unsolicited emails to our social media feed, to the nightly news report inundates us with shock, confusion, and consternation. Modern media has been documented to decrease the capacity for concentration, discipline, and the kind of work ethic necessary to thrive in the modern professional sector.22
Almost any wild mammal placed in a nightclub or movie theater would frantically try to escape. Ironically, these are the places we go to relax even though our innate senses want to retreat from loud sounds, bright lights, and quick movement. They keep our amygdala ringing with fear. Even children’s movies today are hysterically paced and feature constant calamity and pandemonium. A large proportion of children are incapable of breathing through their noses under these conditions. As we sit consuming popular media, we hyperventilate, sneer, startle, raise our eyebrows, brace our vocal cords, and protract our necks. As long as you allow media content to impede your breathing pattern, this is inescapable.

When the diaphragm tenses, it is like a turtle retreating into its shell. It “wants to hide” from loud sounds and fast movement. When it is afraid, it lies still in partial contraction. When it feels safe it ventures out. While we consume entertainment media our tendency is to breathe with the chest and freeze the diaphragm in place. The diaphragm remains buried inside the rib cage like the turtle’s head inside its shell. This keeps the belly still. During each inhalation, pay attention to the downstroke of your diaphragm. Imagine it emerging from the bottom of your ribs and pushing on the contents of your belly. As you perform Activity 21.3 above, you should have dozens of breakthrough moments where, little by little, you are able to encourage your diaphragm to come out and play.
As with drug use, intense stimulation from modern media causes us to completely disregard the panic signals our body is sending us. Performing paced breathing while engaging in these activities is an excellent way to learn to retain your composure as you are inundated. If you practice, you will get to the point where you can breathe through your nose at five breaths per minute in a loud theater, digital firefight, or clamoring nightclub for hours at a time. Allow me to point out that it doesn’t matter which arena, arcade, or bar you are in; if you breathe at five breaths per minute or less, you are automatically the coolest cat there.
Most video games create suspenseful situations in which players must react quickly to keep their character from being hurt or killed. The simulated danger and time pressure recruits fast-acting areas of the brain, such as the amygdala and basal ganglia, to help perform the hazardous button pressing. These unconscious brain areas don’t know they are just being recruited to play a game. They assume the actions are dire, and so involuntarily activate the sympathetic system. This is why playing real-time video games can be affectively detrimental. Each decrement in the character’s life bar causes startle and cortisol release.23 Each startle contributes ever so slightly to one’s background hum of anxiety. Moreover, as you hold the controller (as with your phone or keyboard), most of your major postural muscles are completely braced and immobilized. In a very real sense, we are monkeys being terrorized while handcuffed to the keyboard, mouse, or controller.
Videogames have been shown to increase cortisol levels, bolster aggressive affect, and reduce prosocial behavior.24 Most of my friends who play video games act breathless and panicked afterward, driving them to smoke cigarettes and drink alcohol during gaming breaks. Playing an hour of competitive, online “deathmatches” would strip almost anyone of their composure. Over time, this undermines autonomic balance. In my twenties I didn’t realize that loud, violent entertainment was turning me into the stereotype of the high-strung geek.
Many studies have shown that merely reducing television volume can vastly reduce the sympathetic stress response to violent videos and games. In general, the louder the TV, the more frequently and intensely the amygdala is triggered, and the more cortisol is released. Turn your speakers down a few decibels, and you should notice that you feel far less uneasy after a play session or an action movie. We should also seek out activities that put us into a state of flow and stimulate dopamine without stimulating cortisol. What you are doing right now, reading, may be one of the best. Socialization, meditation, massage, sex, singing, and exercise are others.
Some breathtaking things are good for us. But we need to differentiate between the scenic overlook and addictive trauma. Overstimulating media tricks our bodies into thinking we are preparing for tremendous amounts of exercise, even though we usually consume it while sitting on our backsides. Rather than stewing in them, use up your stress hormones by engaging in physical activity.
Conclusion: Exercise Is the Best Antistress Tool
Perhaps the best antidote for stress is regular exercise. There is an extensive body of research documenting the many benefits. Exercise bolsters self-esteem, enhances body image, increases stress resilience, and is an effective treatment for depression and anxiety.25 Some studies indicate that exercise may even increase life expectancy and the overall quality of life.26 There are many reasons to exercise.
Health Benefits of Exercise
- Improves circulation efficiency and reduces blood pressure
- Increases pain tolerance
- Increases the number of red blood cells, facilitating oxygen transport
- Lowers total cholesterol while raising good cholesterol
- Prevents bone loss and stimulates bone growth reducing the risk of osteoporosis
- Promotes weight loss
- Reduces risk for heart disease, blood clots, and stroke
- Reduces the risk for diabetes and cardiovascular issues
- Strengthens the heart muscle, improves its efficiency, and reduces resting heart rate
- Strengthens the muscles of respiration
Most people don’t engage in daily physical activity because it feels uncomfortable. They assume exercise will add to their distress. It’s true: exercise does lead to a slight increase in adrenaline and cortisol. This is why we must appraise the sensation of exercise as positive stress, a challenge, and as under our control. Moreover, mounting a small stress response to exercise repeatedly will diminish your stress response to subsequent exercise. In other words, the more you train, the less uncomfortable it becomes.
Exercise involves the good type of stress that fortifies us against bad types. It does this by teaching the respiratory and cardiovascular systems how to handle heavy loads and recover rapidly. Also, after exercise, stress plummets. For instance, it is known that blood concentration levels of cortisol rebound (fall off) abruptly. On the other hand, cortisol rebound after social stress is sluggish and it won’t rebound at all if it leads to rumination. The next time you find yourself overthinking an argument, take a run. You may find it wipes most of your concerns away.
Exercise is a potent antidepressant and anxiolytic that makes us feel significantly less affected by unfavorable events. The reason is that physical exertion, whether aerobic or anaerobic, results in endorphin release. Beta-endorphin is a neurohormone released into the bloodstream from the pituitary gland during exercise.27 Endorphins attach themselves to specific receptor sites in the brain that affect our perception of well-being and, in large amounts, can even create the feeling of euphoria. Endorphins are the body’s way of rewarding us for exerting ourselves. Endorphins not only give you a sense of pleasure; they also suppress appetite, elevate mood, increase memory retention, and improve immune activity.28
Aerobic exercise results in the increased creation of new brain cells (neurogenesis) in the same areas that lose cells in people with depression (such as the hippocampus). The concentration of nerve growth factors, like GDNF and BDNF, increases with exercise. These proteins cause neuron branches to grow and make new connections. They also reduce susceptibility to degeneration. It is no wonder that a sedentary lifestyle is a risk factor for neurodegenerative illnesses in humans. If you don’t exercise to improve health, fitness, or appearance, then do it to increase the quality of your level of consciousness. In fact, exercise has many positive biological effects on the brain.
Neurobiological Effects of Exercise
- Boosts energy and reduces stress
- Improves brain structural connections
- Improves cognitive function, cognitive control, and various forms of memory
- Improves mental health, increasing cognitive capacity
- Improves mental wellness by relieving stress, tension, anxiety, and depression
- Improves self-image and confidence
- Improves sleep quality
- Increases gray matter density
- Results in new neuron growth
Exercise enhances the feel-good neuromodulators while having none of the downsides of overeating, drugs, alcohol, or chaotic entertainment. The endorphin release that occurs during exercise is one reason why running around the block once or twice can make you come across as highly relaxed before a meeting, date, or party. The other reason is that it resets the level of tension in your chest.
Unspent, negative energy will inevitably be funneled toward the bracing of your diaphragm. This makes it so that a tense “claw” powers each inhalation and exhalation. Intense cardiovascular exercise that requires heavy breathing forces you to loosen that claw and expand the diaphragm’s range simply so that you can get enough air. Additionally, when an exercise thoroughly works out your breathing musculature, it will need rest, preventing it from reverting to its usual pattern of heavy tension. In other words, aerobic exercise stimulates and strengthens the breathing musculature, making it largely incompatible with bracing the diaphragm.

Wolves and wild dogs often travel tens of miles daily while foraging. They are designed for sustained, daily activity. Dog trainers know that daily exercise is the most important aspect of rehabilitating problem dogs. This is because being deprived of activity without an outlet for their natural energy increases neurotic, defiant, and aggressive behaviors. Dismally, many people don’t bother to walk their dogs. Professionals dog behaviorists like Cesar Millan argue that walking a dog for less than sixty minutes every day is abusive.29 Millan walks his dogs in a large pack for at least four hours a day. He doesn’t do this for their physical health as much as their mental health. How much exercise is enough for humans? It isn’t clear, but many experts and the U.S. Department of Health and Human Services recommend at least 20 minutes of moderate aerobic activity every day. I would say that we should shoot for more like 40.
You need a daily outlet for your natural energy just as much as any other mammal. Every day you skip cardiovascular exercise, you are mismanaging your body and compounding your stress, social defeat, and pain. To stay motivated, make your workouts fun, varied and (as discussed in Chapter 15) not too strenuous. Listen to an audiobook, a podcast, or your favorite music. Become interested in and build skill at as many different forms of exercise as you can. Try out different sports, gymnasiums, and classes in your neighborhood (see table below). Ask your friends if you can join them in their routines. Dance and practice yoga every day. Lift weights using the anti-laxity and anti-rigidity techniques. Get out for a walk using the exercises in Chapter 17. Free yourself from that self-imposed kennel.
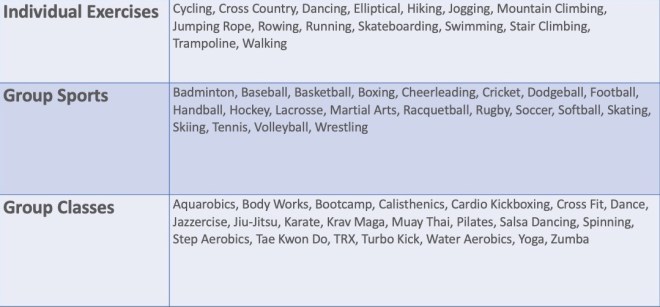
Table 21.1: Forms of cardiovascular and aerobic exercises to try.
Chapter Twenty-One: Bullet Points
- Don’t fear stress. Apprehension of stress makes it more physiologically detrimental.
- We can respond to stressors in a healthy way by considering them challenges (challenge response) or in an unhealthy way by considering them threats (threat response).
- Whether your unconscious mind responds to stressors with the threat response or the challenge response may be determined by the quality of your breathing.
- Virtually all drug use leads to withdrawal symptoms that weaken you as a person.
- People who mix socializing with drugs unknowingly brace various muscles and organs for sustained periods.
- Video games, loud music, and violent, suspenseful entertainment lead to low-level panic that can become chronic.
- You are on “no chill” mode. And you need to come off it.
- Consider taking one day a week, perhaps Sundays, to unwind and remove yourself from all worries, work, rushes, and social conflicts. A whole day of rest serves as a “macrobreak.” Committing 1/7 of your life to restorative relaxation can make a huge difference over time.
- Regular exercise releases endorphins and enhances our mood, keeping our minds from running our bodies into the ground.
- Anxiety is your body’s way of begging you for exercise.
Endnotes
- Ellis, B. J., Jackson, J. J., & Boyce, W. T. (2006). The stress response systems: Universality and adaptive individial differences. Developmental Review, 26, 175-212.
- Wingfield, J. C., Donna L. Maney, Creagh W. Breuner, Jacobs, J. D., Sharon Lynn, Ramenofsky, M., & Ralph D. Richardson. (1998). Ecological bases of hormone-behavior interactions: The “Emergency Life History Stage.” American Zoologist, 38(1), 191–206.
- Marks, I., & Nesse, R. (1994). Fear and fitness: An evolutionary analysis of anxiety disorders. Ethology and Sociobiology, 15(5), 247-261.
- Miller, D. B., & O’Callaghan, J. P. (2002). Neuroendocrine aspects of the response to stress. Metabolism: Clinical and Experimental, 51(6 Suppl 1), 5–10; Sapolsky, R. M., Krey, L. C., & McEwen, B. S. (1986). The neuroendocrinology of stress and aging: The glucocorticoid cascade hypothesis. Endocrine Reviews, 7(3), 284–301; Lovallo, W. R., & Gerin, W. (2003). Psychophysiological reactivity: Mechanisms and pathways to cardiovascular disease. Psychosomatic Medicine, 65(1), 36-45.
- LeDoux, J. (1996). The emotional brain: The mysterious underpinnings of emotional life. Simon and Schuster.
- Bremner J. D. (1999). Does stress damage the brain? Biological Psychiatry, 45(7), 797–805; LeDoux, J. (1998). Fear and the brain: Where have we been, and where are we going? Biological Psychiatry, 44(12), 1229-1238.
- LeDoux, J. (2015). Anxious: Using the brain to understand and treat fear and anxiety. Penguin Books.
- Sapolsky, R. M. (2017). Behave: The biology of humans at our best and worst. Penguin Press.
- Sapolsky, R. M. (2005). The influence of social hierarchy on primate health. Science, 308(5722), 648–652.
- Sapolsky, 2017, Behave: The biology of humans at our best and worst.
- Sapolsky, R. M., Romero, L. M., & Munck, A. U. (2000). How do glucocorticoids influence stress responses? Integrating permissive, suppressive, stimulatory, and preparative actions. Endocrine Reviews, 21(1), 55–89.
- Nelson, E. E., & Winslow, J. T. Non-human primates: Model animals for developmental psychopathology. Neuropsychopharmacology, 34(1), 90–105.
- McGonigal, K. (2015). The upside of stress: Why stress is good for you and how to get good at it. Penguin Random House.
- Brooks, A. (2013). Get excited: Reappraising pre-performance anxiety as excitement. Journal of Experimental Psychology, 143(3), 1144 –1158.
- McGonigal, 2015, The upside of stress:Why stress is good for you and how to get good at it.
- Glass, D. C., Reim, B., & Singer, J. E. (1971). Behavioral consequences of adaptation to controllable and uncontrollable noise. Journal of Experimental Social Psychology, 7(2), 244–257; Minor, T. R., Jackson, R. L., & Maier, S. F. (1984). Effects of task-irrelevant cues and reinforcement delay on choice-escape learning following inescapable shock: evidence for a deficit in selective attention. Journal of Experimental Psychology: Animal Behavior Processes, 10(4), 543–556.
- Sapolsky, R. M. (1994). Why zebras don’t get ulcers. Henry Holt and Company.here.
- Gude, D. (2012). Hair loss: A harbinger of morbidities to come! International Journal of Trichology, 4(4), 287–288.
- Testino, G., Leone, S., & Borro, P. (2014). Treatment of alcohol dependence: Recent progress and reduction of consumption. Minerva Medica, 105(5), 447–466.
- Elliott, S., & Edmonson, E. (2006). The new science of breath: Coherent breathing for autonomic nervous system balance, health, and well-being. Coherence Press.
- Sanchis-Gomar, F., Pareja-Galeano, H., Cervellin, G., Lippi, G., & Earnest, C. P. (2015). Energy drink overconsumption in adolescents: implications for arrhythmias and other cardiovascular events. Canadian Journal of Cardiology, 31(5), 672–575.
- Christakis, D. A., Ramirez, J. S. B., Ferguson, S. M., Ravinder, S., & Ramirez, J. (2018). How early media exposure may affect cognitive function: A review of results from observations in humans and experiments in mice. PNAS, 115(40), 9851–9858.
- Gentile, D. A., Bender, P. K., & Anderson, C. A. (2017). Violent video game effects on salivary cortisol, arousal and aggressive thougthts in children. Computers in Human Behavior, 70, 39–43.
- Anderson, C. A., & Bushman, B. J. (2001). Effects of violent video games on aggressive behavior, aggressive cognition, aggressive affect, physiological arousal, and prosocial behavior: A meta-analytic review of the scientific literature. Psychological Science, 12(5), 353–359.
- Babyak, M., Blumenthal, J. A., Herman, S., Khatri, P., Doraiswamy, M., Moore, K., & Krishnan, K. R. (2000). Exercise treatment for major depression: Maintenance of therapeutic benefit at 10 months. Psychosomatic Medicine, 62(5), 633–638.
- Gremeaux, V., Gayda, M., Lepers, R., Sosner, P., Juneau, M., & Nigam, A. (2012). Exercise and longevity. Maturitas, 73(4), 312–7.
- Boecker, H., Sprenger, T., Spilker, M. E., Henriksen, G., Koppenhoefer, M., Wagner, K. J., Valet, M., Berthele, A., & Tolle, T. R. (2008). The runner’s high: opioidergic mechanisms in the human brain. Cerebral Cortex, 18(11), 2523–2531.
- Anderson, E., & Shivakumar, G. (2013). Effects of exercise and physical activity on anxiety. Frontiers in Psychiatry, 4, 27.
- Millan, C., & Peltier, M. J. (2006). Cesar’s way: The natural, everyday guide to understanding & correcting common dog problems. Random House.
